Welcome to
Kauai Dental Care
We’ve been the trusted dentists of Lihue-area families for over 30 years! We believe in building genuine, long-lasting relationships through open and honest communication.
Dentistry when you need it
Dental Care from the First Tooth
A Beautiful Smile is a Youthful Smile
Oral & Overall
Health Connected
We Are Kauai Dental Care
Dr. Ing and Dr. Park
are accepting new patients!
With more than 30 years of providing dental care to our family and friends on Kauai, you can count on us to be here for you and your family for many years to come.
If you’re new to Kauai and looking for an office that is professional, respects your time, and cares about both your oral health and overall health, then give us a call! Our team takes care of the dental health needs of children and adults.

Alan Ing, DDS

Yun Park, DDS

What Kauai Dental Care Patients Are Saying!
Testimonials
About Kauai Dental Care
Professional, Knowledgeable, Experienced
From check-in, throughout your treatment, until check-out, your experience should be smooth, efficient, informative, and comfortable. You’ll experience this with our trained and knowledgeable team.
Fun, Warm, Caring
Do you love your hygienist? Everyone on our team is unique & awesome in their own way – quiet, gentle, energetic, funny, kind, or down-to-earth. Let us know who you would prefer!
Gentle, Skilled, Friendly
Dr. Ing and Dr. Park have established a strong reputation for gentle, quality dental care on Kauai where they have been caring for generations of family members for over 30 years.
Clean, Safe, State-of-the-Art
Having the latest, tried-and-true technology, in both the front and back office, improves the efficiency of your visit, minimizes the pain, and provides a more comfortable experience.

New DENTAL Patient?
Kauai Dental Care
Featured Dental Services
Having the latest, tried-and-true technology, in both the front and back office, improves the efficiency of your visit, minimizes the pain, and provides a more comfortable experience.

Same-Day Crowns
Getting a crown used to mean multiple office visits, but now there is a much more convenient option – same-day crowns.

Dentures
It is important to get the best type of dentures to suit your lifestyle. The two main types of dentures are Partial Dentures and Full Dentures.
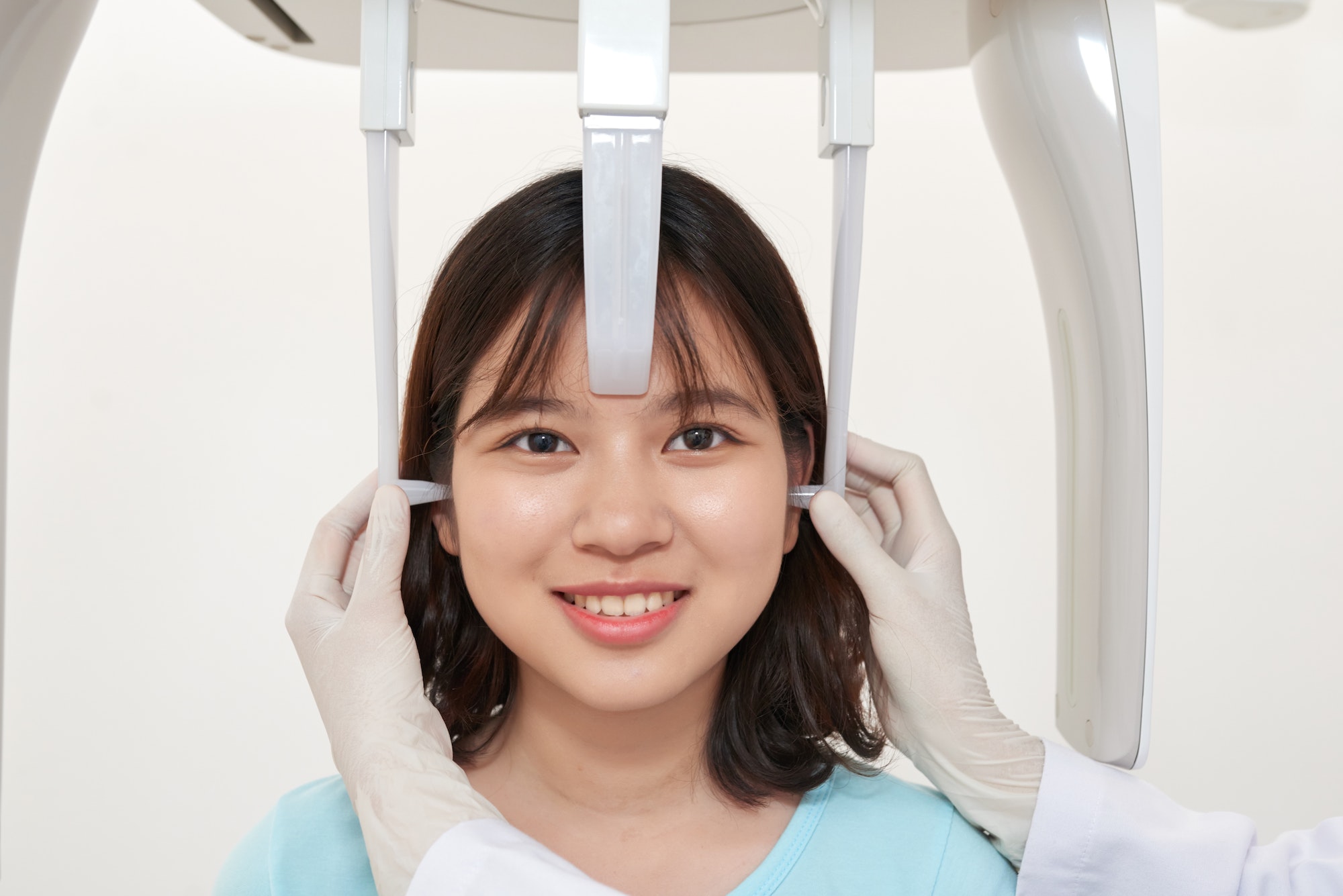
Digital X-Rays
X-rays are one of the most important parts of a dental exam, and can help detect problems long before they are visible to the naked eye.
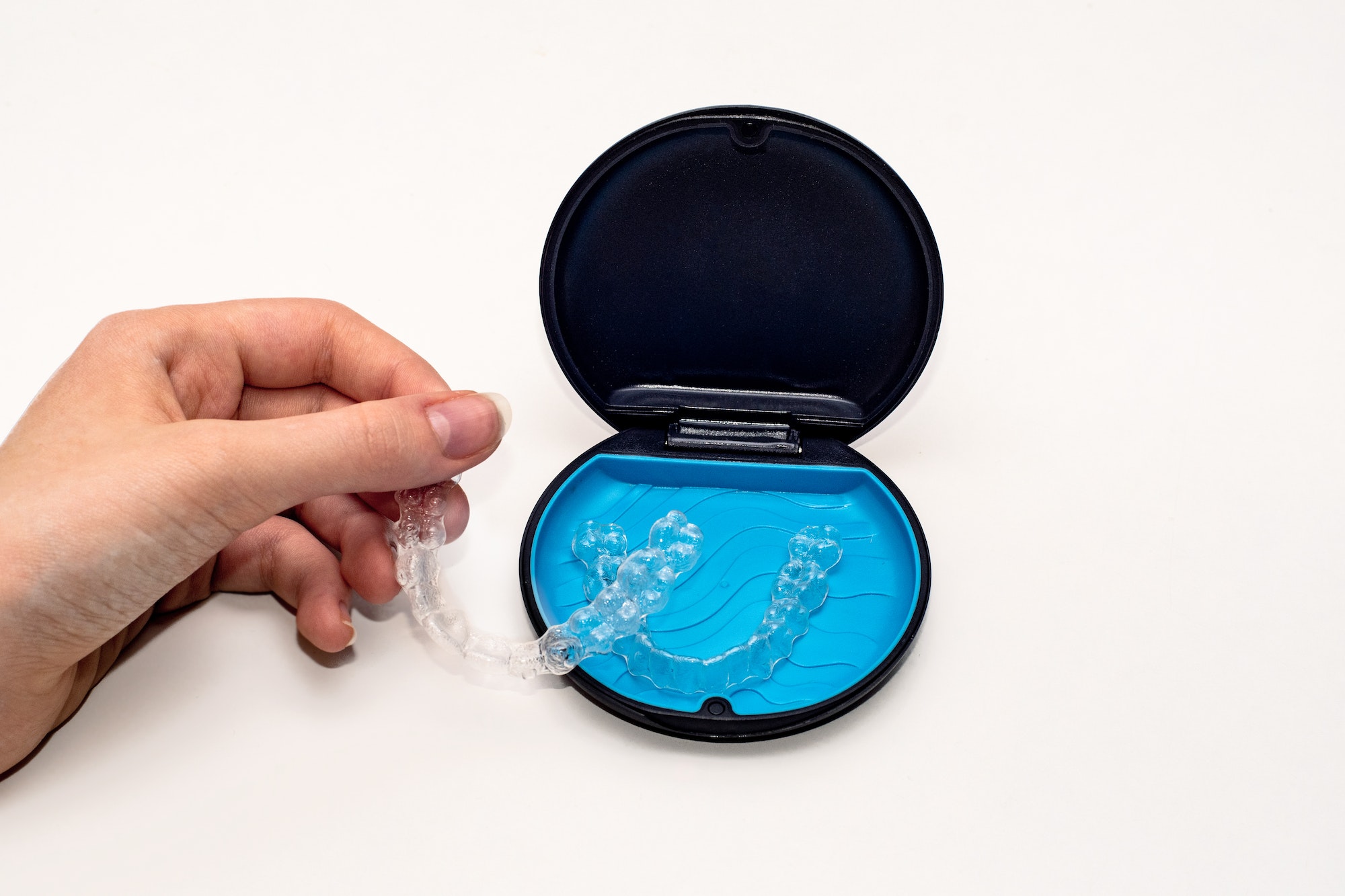
Invisalign
A modern approach to orthodontics, invisalign is a virtually invisible solution, custom-made to straighten your teeth.

Veneers
Our veneers are expertly designed to enhance your smile by correcting color, shape, and spacing issues for a natural-looking result.
About Our Practice
Ever said to yourself, I wish I had a dentist in the family? Many of our patients have been coming to see us since we opened! As we get to know you and your mouth, you will get to know us too! Just like a having a dentist in the family, once we get to know you, we’ll be just one call away.